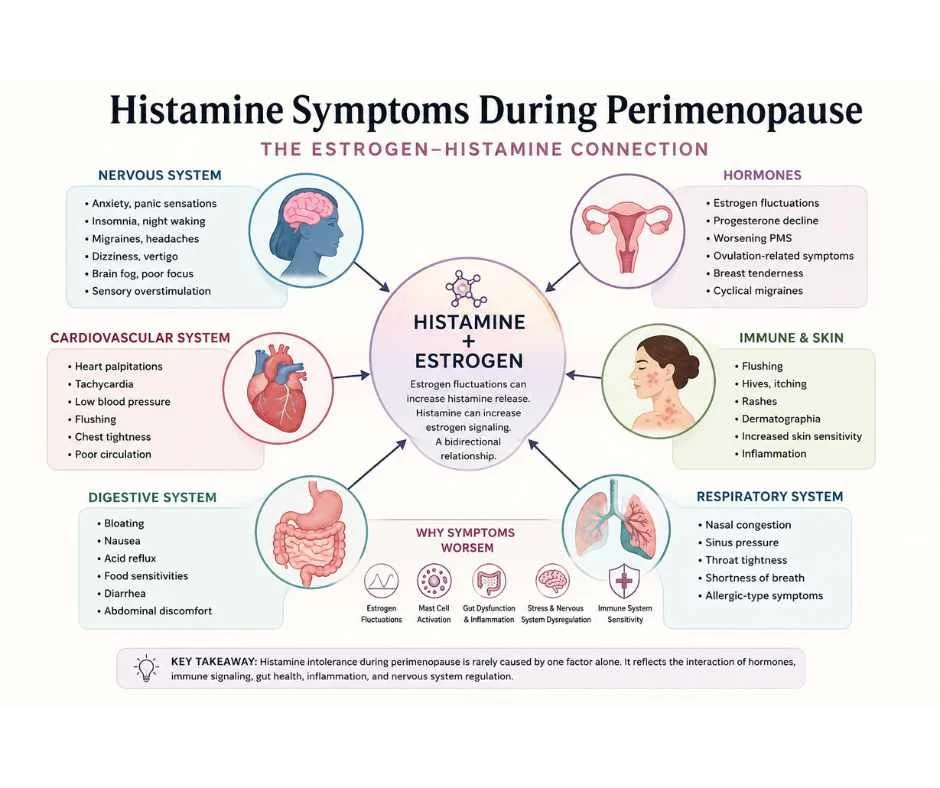
Histamine Intolerance During Perimenopause: How Estrogen Affects Histamine Symptoms
Why Histamine Intolerance Often Gets Worse During Perimenopause
Many women entering perimenopause suddenly begin experiencing symptoms that seem disconnected at first: flushing, migraines, insomnia, anxiety, dizziness, heart palpitations, food sensitivities, itching, sinus congestion, worsening PMS, skin reactions, or unexplained inflammatory symptoms. In many cases, these patterns may involve a deeper interaction between estrogen fluctuations, histamine regulation, mast cell activation, gut dysfunction, inflammation, and nervous system stress. Many women feel confused when symptoms appear suddenly despite eating well, exercising, and being told their labs are normal.
Perimenopause is not simply a reproductive transition. It is a period of major neuroendocrine, immune, and metabolic change involving fluctuating estrogen levels, declining progesterone, altered cortisol signaling, changing gut microbiome composition, increased inflammatory burden, and reduced physiologic resilience. These shifts may create conditions in which histamine becomes more difficult for the body to regulate effectively. (1) This is one reason histamine intolerance during perimenopause may emerge even in women who previously tolerated foods, stress, or hormonal fluctuations without major symptoms.
For some women, this may present as histamine intolerance. For others, symptoms may involve mast cell activation, impaired histamine breakdown, estrogen dominance patterns, gut permeability, chronic inflammatory signaling, or combinations of multiple overlapping physiologic stressors.
Importantly, many women experiencing histamine symptoms during perimenopause are told their hormone labs are “normal,” despite ongoing symptoms involving sleep, anxiety, skin reactivity, digestion, migraines, and nervous system overstimulation. Histamine-related patterns are frequently multifactorial and may not be identified through standard evaluations alone.
This article discusses the connection between estrogen and histamine during perimenopause, why histamine symptoms may worsen during hormonal transitions, and how a root-cause, systems-based approach may help support hormonal, immune, gut, and nervous system regulation.
What Is Histamine Intolerance in Perimenopause?
Histamine intolerance during perimenopause refers to a pattern in which fluctuating estrogen levels, declining progesterone, mast cell activation, gut dysfunction, inflammation, and impaired histamine breakdown contribute to symptoms such as flushing, headaches, anxiety, insomnia, food sensitivities, palpitations, itching, digestive symptoms, and skin reactions. Symptoms often worsen during hormonal fluctuations because estrogen and histamine influence each other bidirectionally. (2)
Histamine itself is not inherently harmful. Histamine is a normal biologically active compound involved in:
Immune signaling
Neurotransmitter function
Stomach acid production
Circadian rhythm regulation
Vascular tone
Inflammatory responses
Problems arise when histamine accumulation exceeds the body’s ability to break it down efficiently.
Many women tolerate small amounts of histamine individually but react once cumulative histamine load exceeds their physiologic threshold.
Common Signs of Histamine Intolerance During Perimenopause
Flushing
Anxiety
Insomnia
Food sensitivities
Migraines
Heart palpitations
Itching
Hives
Nasal congestion
Dizziness
Worsening PMS
Common Histamine Symptoms During Perimenopause
Histamine intolerance during perimenopause can affect multiple body systems simultaneously.
Neurologic and Nervous System Histamine Symptoms
Anxiety
Panic sensations
Insomnia
Racing thoughts
Brain fog
Migraines
Dizziness
Sensory overstimulation
Heart palpitations
Skin and Immune-Related Histamine Symptoms
Flushing
Hives
Itching
Rashes
Dermatographia
Increased skin sensitivity
Digestive Symptoms of Histamine Intolerance
Bloating
Nausea
Acid reflux
Food sensitivities
Diarrhea
Abdominal discomfort
Respiratory Histamine Symptoms
Nasal congestion
Sinus pressure
Throat tightness
Shortness of breath
Hormonal Symptoms Linked to Histamine and Estrogen
Worsening PMS
Heavy periods
Breast tenderness
Ovulation-related symptoms
Cyclical migraines
Increased symptoms before menstruation
Many women notice histamine symptoms worsen during ovulation, the late luteal phase, or the irregular hormonal fluctuations common during perimenopause. (3)
How Estrogen and Histamine Affect Each Other
One of the most important aspects of histamine intolerance during perimenopause is the bidirectional relationship between estrogen and histamine.
Estrogen Can Increase Histamine Release
Estrogen can stimulate mast cells to release histamine. Mast cells are immune cells found throughout connective tissue, digestive tissue, the skin, sinuses, blood vessels, and the nervous system. (4)
As estrogen rises or fluctuates unpredictably, histamine release may increase in susceptible individuals.
Histamine Can Increase Estrogen Signaling
Histamine can also stimulate ovarian estrogen production and influence estrogen signaling pathways. This can create a physiologic amplification loop:
Estrogen increases histamine release
Histamine increases estrogen signaling
Increased estrogen further activates mast cells
Histamine burden escalates further
This may partially explain why histamine intolerance symptoms often worsen during hormonal fluctuations, estrogen dominance patterns, or perimenopause transitions. (5)
→ Hormone & Metabolic Optimization
Root Causes of Histamine Intolerance During Perimenopause
Histamine intolerance during perimenopause is rarely caused by one factor alone. More commonly, it reflects overlapping physiologic stressors affecting immune, hormonal, digestive, metabolic, and nervous system regulation simultaneously.
Estrogen Fluctuations
Perimenopause often involves unstable estrogen signaling rather than simply low estrogen. Rapid hormonal fluctuations may increase mast cell activation and histamine release.
Progesterone Decline
Progesterone commonly declines before estrogen during perimenopause. Progesterone has stabilizing effects on the nervous system and mast cells. As progesterone falls relative to estrogen, histamine-related symptoms may intensify. (6)
Mast Cell Activation
Mast cells release histamine along with inflammatory mediators including cytokines, prostaglandins, leukotrienes, and tryptase. Mast cell activation may be triggered by:
Stress
Hormonal fluctuations
Mold exposure
Infections
Environmental toxins
Heat
Alcohol
Sleep deprivation
Gut inflammation
Gut Dysfunction
The gastrointestinal tract plays a major role in histamine metabolism and estrogen clearance.
DAO (diamine oxidase), one of the primary enzymes involved in dietary histamine breakdown, is produced largely in the intestinal lining. Gut inflammation and intestinal permeability may impair DAO production and histamine regulation. (7)
Certain bacterial strains may also produce histamine directly, increasing histamine burden further.
Impaired Estrogen Clearance
The gut microbiome influences estrogen metabolism through the estrobolome, bacterial populations involved in estrogen processing and recirculation. Dysbiosis may contribute to impaired estrogen clearance and prolonged estrogen exposure. (8)
Chronic Stress and Cortisol Dysregulation
Histamine regulation is closely tied to the nervous system. Chronic sympathetic activation and cortisol dysregulation may increase inflammatory signaling, mast cell activation, and histamine release.
Many women entering perimenopause are simultaneously navigating:
Sleep disruption
Chronic stress
Blood sugar instability
Overtraining
Under-recovery
Caregiver burden
Chronic inflammation
Environmental toxic burden
Over time, these stressors may reduce physiologic resilience and increase histamine sensitivity.
Why Histamine Symptoms During Perimenopause Often Feel Like Anxiety
Histamine functions not only as an immune compound but also as an excitatory neurotransmitter within the brain and nervous system.
Elevated histamine activity may contribute to:
Hypervigilance
Panic sensations
Night waking
Adrenaline surges
Racing thoughts
Sensory overstimulation
Feeling “wired but exhausted”
This overlap is one reason histamine intolerance during perimenopause is sometimes mischaracterized as purely psychological or stress-related.
Histamine-related anxiety patterns may become especially noticeable during hormonal shifts involving estrogen fluctuations and declining progesterone levels.
How Gut Health Affects Histamine Intolerance During Perimenopause
Gut dysfunction is one of the most common contributors to histamine intolerance during perimenopause.
Potential contributors may include:
Dysbiosis
Intestinal permeability
Chronic inflammation
Reduced DAO activity
Food sensitivities
Impaired digestion
Altered microbiome diversity
Chronic stress physiology
Histamine issues frequently overlap with broader inflammatory gut patterns affecting immune signaling, estrogen metabolism, nutrient absorption, and nervous system regulation simultaneously.
→ Gut Health & Digestive Restoration
High-Histamine Foods That May Trigger Symptoms
Histamine tolerance thresholds vary considerably between individuals.
Common higher-histamine foods include:
Wine and alcohol
Fermented foods
Aged cheeses
Processed meats
Vinegar
Kombucha
Leftovers
Canned fish
Smoked foods
Tomatoes
Spinach
Avocado
Some foods may also trigger histamine release despite not containing large amounts of histamine themselves.
Long-term restrictive dieting is not always appropriate. In many cases, the broader goal is improving histamine resilience and reducing overall inflammatory burden rather than permanently eliminating large categories of foods.
Nutrient Deficiencies That May Affect Histamine Regulation
Histamine metabolism depends on multiple nutrient-dependent pathways involving detoxification, methylation, antioxidant protection, and enzymatic function.
Potential contributors may include deficiencies involving:
Vitamin B6
Magnesium
Copper
Zinc
Vitamin C
Riboflavin
Folate
Histamine metabolism may also intersect with methylation pathways involving COMT activity, HNMT pathways, oxidative stress regulation, and mitochondrial function. (9)
Why Conventional Testing Often Misses Histamine-Related Symptoms
Histamine intolerance during perimenopause can be difficult to identify through conventional testing alone.
Several factors contribute to this:
Histamine symptoms fluctuate significantly
DAO testing has limitations
Mast cell activation patterns may not appear consistently on labs
Symptoms often overlap with anxiety, menopause, IBS, migraines, or allergic conditions
Standard hormone testing may miss dynamic hormonal fluctuations
Nervous system dysregulation may not appear on routine evaluations
Many women therefore experience years of symptoms despite repeatedly being told that testing appears “normal.”
A systems-based approach evaluates how hormonal fluctuations, gut health, inflammation, nervous system regulation, immune signaling, environmental exposures, and metabolic function may be interacting simultaneously.
→ Advanced Functional Lab Testing
A Root-Cause Functional Medicine Perspective on Histamine Intolerance During Perimenopause
At Denver Sports & Holistic Medicine, histamine-related symptoms are evaluated through a broader systems-based framework that considers hormone fluctuations, gut health, nervous system regulation, inflammation, immune signaling, detoxification capacity, and environmental contributors simultaneously.
A comprehensive evaluation may involve assessing:
Hormone patterns
Estrogen metabolism
Progesterone balance
Gut function
Dysbiosis
Intestinal permeability
Chronic inflammation
Mast cell activation patterns
Nervous system regulation
Sleep physiology
Nutrient status
Blood sugar regulation
Environmental toxic burden
Histamine intolerance during perimenopause is often not an isolated food issue alone. More commonly, it reflects broader physiologic dysregulation involving multiple interconnected systems.
Conventional approaches often focus primarily on antihistamines or symptom suppression, whereas a systems-based functional medicine approach evaluates why histamine regulation became dysregulated in the first place.
→ Acupuncture & Nervous System Regulation
How to Support Histamine Intolerance During Perimenopause Naturally
Supportive strategies should be individualized based on the underlying physiologic patterns involved.
Potential approaches may include:
Nervous System Support
Sleep optimization
Breathwork
Acupuncture
Stress reduction
Circadian rhythm support
Gut Restoration Support
Supporting gut barrier integrity
Addressing dysbiosis
Improving digestive function
Reducing inflammatory triggers
Hormone Support
Supporting estrogen metabolism
Evaluating progesterone balance
Addressing insulin resistance and metabolic dysfunction
Nutritional Strategies
Temporary low-histamine nutrition approaches when appropriate
Blood sugar stabilization
Anti-inflammatory dietary support
Environmental Medicine Approaches
Mold evaluation
Reducing toxic burden
Supporting detoxification pathways
The goal is not simply suppressing symptoms temporarily, but improving physiologic resilience and reducing the upstream drivers contributing to histamine dysregulation.
A Systems-Based Approach to Histamine Intolerance During Perimenopause
Histamine intolerance during perimenopause often reflects a broader interaction between hormones, immune signaling, inflammation, gut health, detoxification pathways, mast cell activity, and nervous system regulation rather than a single isolated food sensitivity alone.
For many women, symptoms such as anxiety, insomnia, flushing, migraines, food sensitivities, palpitations, itching, and inflammatory reactions may emerge gradually as physiologic resilience declines during hormonal transition years. These symptoms are frequently multifactorial and may involve overlapping patterns related to estrogen fluctuations, progesterone decline, chronic stress, gut dysfunction, mast cell activation, inflammation, and environmental burden.
Because histamine symptoms can mimic anxiety disorders, menopause symptoms, allergic reactions, digestive conditions, or inflammatory syndromes, many women spend years searching for answers despite being told that standard testing appears normal.
A systems-based functional medicine approach focuses on identifying the upstream physiologic patterns contributing to histamine dysregulation rather than simply suppressing symptoms temporarily. Supporting histamine regulation often requires addressing the broader physiologic environment influencing hormones, inflammation, gut health, immune signaling, detoxification pathways, and nervous system resilience simultaneously.
You may request a free 15-minute consultation with Dr. Martina Sturm to review your health concerns and outline appropriate next steps within a root-cause, systems-based framework.
Frequently Asked Questions About Histamine Intolerance During Perimenopause
Can perimenopause cause histamine intolerance?
Perimenopause may contribute to histamine intolerance due to fluctuating estrogen levels, declining progesterone, mast cell activation, gut dysfunction, inflammation, and nervous system stress that affect histamine regulation.
Why do histamine symptoms worsen before a period?
Histamine symptoms may worsen before a period because hormonal fluctuations involving estrogen and progesterone can influence mast cell activation and histamine release.
Can estrogen increase histamine levels?
Estrogen may stimulate mast cells to release histamine, while histamine may also influence estrogen signaling pathways, creating a bidirectional relationship between estrogen and histamine.
Can histamine intolerance cause anxiety during perimenopause?
Elevated histamine activity may contribute to anxiety, insomnia, hypervigilance, adrenaline surges, palpitations, and nervous system overstimulation in some women during perimenopause.
Can gut problems worsen histamine intolerance?
Gut dysfunction may impair DAO production, increase inflammatory signaling, alter estrogen metabolism, and contribute to dysbiosis involving histamine-producing bacteria.
Are antihistamines enough to treat histamine intolerance?
Antihistamines may temporarily reduce symptoms for some individuals but may not address upstream contributors such as hormone fluctuations, gut dysfunction, mast cell activation, chronic inflammation, or nervous system dysregulation.
Still Have Questions?
If the topics above reflect ongoing symptoms or unanswered concerns, a brief conversation can help clarify whether a root-cause approach is appropriate.
Resources
Frontiers in Immunology – The Mast Cell, Contact, and Coagulation System Connection in Anaphylaxis
Nutrients – Histamine Intolerance: The Current State of the Art
Journal of Reproductive Immunology – Sex Hormones and Mast Cell Function
Nature Reviews Immunology – Mast Cell Biology
Cells – Estrogen and Histamine Crosstalk
Climacteric – Hormonal Changes During Perimenopause
Nutrients – Diamine Oxidase and Histamine Metabolism
Cell Host & Microbe – The Estrobolome and Estrogen Metabolism
Antioxidants – Oxidative Stress, Mitochondria, and Inflammation