Leaky Gut Syndrome: Causes, Symptoms, and How To Restore Gut Health Naturally
Understanding Intestinal Permeability, Inflammation, and the Root Causes of Chronic Symptoms
Leaky gut syndrome—clinically referred to as increased intestinal permeability—is a systems-level condition that affects far more than digestive health alone. While it originates in the gastrointestinal tract and directly affects gut health, its effects often extend far beyond digestion itself. Many individuals with leaky gut do not initially report classic gut symptoms such as bloating, diarrhea, or abdominal pain.
Instead, early signs frequently present as chronic fatigue, joint or muscle pain, inflammatory skin conditions, allergies, metabolic dysfunction, brain fog, or autoimmune flares. These seemingly unrelated symptoms reflect the gut’s central role in immune regulation, chronic inflammation, metabolic control, and communication with the gut microbiome.
From a functional medicine perspective, this pattern is well recognized. When the intestinal barrier becomes compromised, larger food particles, microbial fragments, and toxins can cross into circulation, triggering immune activation, gut inflammation, and broader systemic inflammation throughout the body. Over time, this dysregulation can strain multiple organ systems—often manifesting far from the digestive tract and long before gastrointestinal symptoms become obvious.
This article explains what leaky gut is, how intestinal permeability develops, why symptoms often appear outside the digestive system, and which root-cause drivers—such as gluten exposure, chronic inflammation, gut microbiome imbalance, immune activation, and environmental stressors—must be addressed to restore gut barrier integrity, digestive health, and whole-body health.
What Is Leaky Gut Syndrome?
Leaky gut syndrome refers to increased intestinal permeability, a condition in which the intestinal lining becomes less effective at regulating what passes from the digestive tract into circulation. When the gut barrier becomes disrupted, inflammatory particles such as bacterial fragments, toxins, and incompletely digested food proteins may cross into the bloodstream and contribute to immune activation, chronic inflammation, food sensitivities, and broader systemic symptoms.
What Is Leaky Gut Syndrome and Intestinal Permeability?
Leaky gut involves dysfunction of the gut barrier system, a complex interface responsible for regulating what is absorbed into circulation and what remains contained within the digestive tract. Under healthy conditions, the intestinal lining functions as a highly selective barrier, allowing nutrients to pass into the bloodstream while preventing bacteria, endotoxins, and incompletely digested food particles from entering systemic circulation.
The gut barrier system is not a single structure, but a complex, multi-layered defense system composed of intestinal epithelial cells, mucus layers, immune signaling molecules, and the gut microbiome. Central to this system are tight junctions—specialized protein complexes that bind adjacent intestinal cells together and dynamically regulate permeability in response to diet, immune signals, microbial activity, and stress (1).
When tight junction integrity is disrupted, permeability increases. This allows larger particles—such as bacterial fragments (including lipopolysaccharides), food antigens, and environmental toxins—to cross the intestinal lining and enter systemic circulation. This process is sometimes described as “leakiness,” but clinically it represents a loss of barrier regulation, not structural damage alone.
Once these particles enter circulation, the immune system identifies them as foreign. Acute immune activation is a normal protective response; however, repeated or ongoing exposure leads to chronic immune stimulation, low-grade systemic inflammation, and progressive immune dysregulation. Over time, this can impair immune tolerance—the ability of the immune system to distinguish harmless substances from true threats—a pattern strongly associated with autoimmune conditions, chronic inflammatory disease, and food sensitivities (1,2).
Importantly, leaky gut is not a standalone diagnosis, but a foundational mechanism that contributes to a wide range of chronic health conditions. Its clinical relevance lies not in the term itself, but in understanding why barrier dysfunction develops, which systems are involved, and how intestinal permeability perpetuates whole-body inflammation. Increasingly, research suggests that gut barrier dysfunction may contribute to immune dysregulation, chronic inflammation, metabolic dysfunction, and broader systemic disease processes throughout the body.
How Increased Intestinal Permeability Develops at the Cellular Level
Increased intestinal permeability develops when inflammatory signaling, microbiome disruption, stress hormones, dietary triggers, or environmental toxins interfere with tight junction regulation within the intestinal lining. As these protective mechanisms weaken, the gut barrier becomes less selective, allowing larger inflammatory particles to enter circulation and stimulate immune activation.
Leaky Gut Symptoms: Why Intestinal Permeability Affects the Entire Body
Approximately 70% of the immune system is associated with the gut, making intestinal barrier integrity central to immune regulation and systemic inflammatory control (2). The gut is not only a digestive organ—it functions as a primary immune interface, continuously sampling what enters the body and determining whether tolerance or defense is required.
When intestinal permeability increases, this regulatory role becomes disrupted. Larger immune-activating particles such as bacterial fragments, endotoxins, and food antigens gain access to circulation, triggering immune signaling far beyond the gut itself. As this exposure persists, several downstream effects can occur:
Inflammatory signaling spreads systemically, shifting the immune system toward chronic low-grade activation
Immune tolerance is impaired, increasing sensitivity to foods, environmental triggers, and self-tissues
Autoimmune activity becomes more likely as regulatory immune pathways are strained
Metabolic and hormonal signaling is affected, as inflammation interferes with insulin sensitivity, thyroid conversion, adrenal regulation, and mitochondrial energy production
Because these effects involve multiple regulatory systems, symptoms often appear in tissues seemingly unrelated to digestion. Joint and muscle pain, respiratory or allergy-type symptoms, inflammatory skin conditions, fatigue, mood or cognitive changes, and immune dysregulation may all reflect gut-driven immune activation—even when gastrointestinal symptoms are mild or absent.
This systemic pattern is one reason leaky gut is frequently overlooked in conventional care: symptoms are evaluated in isolation rather than traced back to a shared regulatory source.
→ Functional & Integrative Medicine
Common Signs and Symptoms of Leaky Gut Syndrome
Leaky gut symptoms often extend far beyond digestion because intestinal permeability affects immune regulation, inflammatory signaling, metabolic function, and nervous system communication throughout the body. While some individuals experience bloating or digestive discomfort, many develop symptoms in seemingly unrelated systems long before gastrointestinal issues become obvious.
Fatigue, Low Energy, and Chronic Exhaustion
Persistent fatigue is one of the most common symptoms associated with leaky gut syndrome. Increased intestinal permeability may contribute to chronic immune activation, inflammatory signaling, nutrient malabsorption, mitochondrial stress, and blood sugar instability, all of which can impair energy production and recovery.
Bloating, Gas, and Digestive Discomfort
Bloating, abdominal pressure, gas, reflux, constipation, diarrhea, and irregular bowel habits are common signs of gut barrier dysfunction and microbiome imbalance. These symptoms may worsen after meals or fluctuate depending on stress, inflammatory foods, or microbial overgrowth.
Food Sensitivities, Inflammation, and Immune Reactivity
As intestinal permeability increases, incompletely digested food particles may cross the gut barrier and trigger immune activation. Over time, this can contribute to delayed food sensitivities, inflammatory reactions, and worsening symptoms after certain foods even when traditional food allergy testing is negative.
Brain Fog, Poor Concentration, and Mood Changes
The gut and brain are closely connected through the gut-brain axis, immune signaling pathways, neurotransmitter production, and the vagus nerve. Chronic inflammation associated with leaky gut may contribute to brain fog, difficulty concentrating, memory issues, anxiety, irritability, and mood dysregulation.
Joint Pain, Muscle Aches, and Chronic Inflammation
Systemic inflammation triggered by intestinal permeability may contribute to joint stiffness, muscle pain, headaches, and generalized inflammatory symptoms. In some individuals, immune activation originating in the gut may aggravate autoimmune or inflammatory conditions affecting connective tissue and musculoskeletal health.
Skin Problems, Eczema, Acne, and Inflammatory Skin Conditions
The gut-skin axis plays a major role in inflammatory skin conditions. Leaky gut and microbiome imbalance may contribute to acne, eczema, rosacea, psoriasis, hives, and other chronic skin symptoms through immune dysregulation and inflammatory signaling.
Autoimmune Symptoms and Immune Dysregulation
Increased intestinal permeability is strongly associated with autoimmune activity and loss of immune tolerance. In genetically susceptible individuals, chronic exposure to inflammatory triggers crossing the gut barrier may contribute to immune dysregulation and autoimmune flare patterns.
Headaches, Migraines, and Nervous System Symptoms
Some individuals with leaky gut experience headaches, migraines, light sensitivity, dizziness, or nervous system hyperreactivity. These symptoms may be linked to inflammatory cytokines, histamine activity, blood sugar instability, microbiome imbalance, and neuroimmune signaling changes.
Hormone Imbalances and Metabolic Dysfunction
Gut barrier dysfunction may influence estrogen metabolism, cortisol regulation, thyroid signaling, insulin sensitivity, and metabolic health. Chronic inflammation originating in the gut can interfere with hormonal communication throughout the body and contribute to broader endocrine dysregulation.
Allergies, Histamine Intolerance, and Sensitivity Reactions
Histamine intolerance, seasonal allergies, chemical sensitivities, sinus congestion, itching, flushing, and exaggerated immune reactions may all be associated with intestinal permeability and microbiome disruption. Because much of the immune system resides in the gut, chronic barrier dysfunction can amplify inflammatory sensitivity patterns over time.
What Causes Leaky Gut Syndrome?
Leaky gut syndrome rarely develops from a single trigger. Instead, increased intestinal permeability typically reflects the cumulative effects of multiple overlapping stressors that impair gut barrier integrity over time (1–4). These factors may disrupt tight junction function, alter microbiome balance, increase inflammatory signaling, weaken immune regulation, and reduce the intestine’s ability to repair and regenerate effectively.
Because the intestinal barrier sits at the intersection of digestion, immunity, metabolism, detoxification, and nervous system regulation, dysfunction in one system often amplifies dysfunction in another. In many individuals, several contributors are active simultaneously, sustaining chronic inflammation and ongoing immune activation.
Gluten, Zonulin, and Intestinal Permeability
Gluten is one of the most extensively studied dietary triggers associated with intestinal permeability. Research shows that gluten may stimulate the release of zonulin, a signaling protein that regulates tight junction function within the intestinal lining. When zonulin activity increases excessively, tight junctions may loosen, allowing inflammatory particles, bacterial fragments, and incompletely digested food proteins to cross into circulation more easily.
This mechanism is well established in celiac disease but may also play a role in non-celiac gluten sensitivity and other inflammatory conditions involving immune dysregulation and gut barrier dysfunction. In susceptible individuals, ongoing gluten exposure may perpetuate chronic inflammation, immune activation, and microbiome disruption even in the absence of overt gastrointestinal symptoms.
Inflammatory Foods and Ultra-Processed Diets
Highly processed diets rich in refined sugars, industrial seed oils, artificial additives, emulsifiers, and low-quality fats may contribute to gut inflammation and microbiome imbalance. These dietary patterns are associated with increased inflammatory signaling, oxidative stress, altered bacterial diversity, and impaired intestinal barrier regulation.
Over time, chronic consumption of inflammatory foods may reduce short-chain fatty acid production, weaken mucus layer integrity, and impair epithelial repair mechanisms that normally protect the gut lining.
Gut Microbiome Imbalance and Dysbiosis
The gut microbiome plays a central role in maintaining intestinal barrier integrity, immune tolerance, nutrient metabolism, and inflammatory regulation. When microbial balance becomes disrupted—a pattern known as dysbiosis—harmful bacteria, fungal overgrowth, or reduced microbial diversity may contribute to increased intestinal permeability.
Microbiome imbalance may reduce production of beneficial compounds such as butyrate, impair immune communication, and increase inflammatory endotoxin exposure within the gut environment. Dysbiosis is frequently associated with antibiotic exposure, poor diet, chronic stress, infections, and environmental toxic burden.
The gut microbiome also plays a major role in digestive health, immune communication, neurotransmitter signaling, and maintenance of the intestinal mucus barrier.
Chronic Stress and Nervous System Dysregulation
Chronic psychological and physiological stress can directly affect intestinal permeability through the gut-brain axis. Elevated cortisol levels, sympathetic nervous system activation, and autonomic imbalance may reduce digestive function, impair gut blood flow, alter microbiome composition, and increase inflammatory signaling within the intestinal lining.
Because the nervous system and immune system communicate closely with the gut, unresolved stress may perpetuate ongoing barrier dysfunction even when dietary interventions are implemented appropriately.
Medications That May Damage the Gut Lining
Certain medications are strongly associated with intestinal barrier disruption and microbiome imbalance. Nonsteroidal anti-inflammatory drugs (NSAIDs), antibiotics, proton pump inhibitors, corticosteroids, and hormonal contraceptives may impair epithelial integrity directly or indirectly through alterations in microbial balance and immune signaling.
Repeated or long-term use of these medications may increase susceptibility to inflammation, dysbiosis, nutrient deficiencies, and chronic gastrointestinal irritation in some individuals.
Environmental Toxins and Mold Exposure
Environmental exposures such as pesticides, glyphosate, heavy metals, mold byproducts, plastics, and air pollutants may contribute to oxidative stress and immune activation at the gut-immune interface. These compounds may impair mitochondrial function, disrupt microbial balance, weaken detoxification pathways, and promote chronic inflammatory signaling throughout the gastrointestinal tract.
In some individuals, chronic environmental exposure becomes a significant contributor to persistent gut inflammation and ongoing intestinal permeability.
Low Vitamin D and Impaired Immune Regulation
Vitamin D plays an important role in immune balance, antimicrobial defense, intestinal barrier maintenance, and inflammatory regulation (3,4). Low vitamin D status has been associated with impaired tight junction integrity, reduced immune tolerance, and increased susceptibility to inflammatory and autoimmune conditions.
Because vitamin D influences both immune signaling and epithelial barrier health, deficiency may contribute to ongoing gut dysfunction and impaired healing capacity.
Autoimmune Predisposition and Genetic Susceptibility
Some individuals may be genetically more susceptible to intestinal permeability and immune dysregulation, particularly when autoimmune conditions run in families. Variations involving immune regulation, inflammatory signaling, detoxification pathways, and microbiome interactions may increase vulnerability to chronic gut inflammation and loss of immune tolerance.
Genetic predisposition alone does not determine disease outcome, but it may lower resilience to environmental, dietary, infectious, and inflammatory stressors that affect gut barrier integrity.
In most cases, leaky gut develops through the interaction of multiple overlapping factors rather than a single isolated cause. For this reason, identifying the primary drivers contributing to ongoing inflammation and barrier dysfunction is often essential for meaningful improvement.
Effective leaky gut treatment depends not on eliminating every possible trigger simultaneously, but on prioritizing the mechanisms most responsible for sustaining intestinal permeability and immune dysregulation.
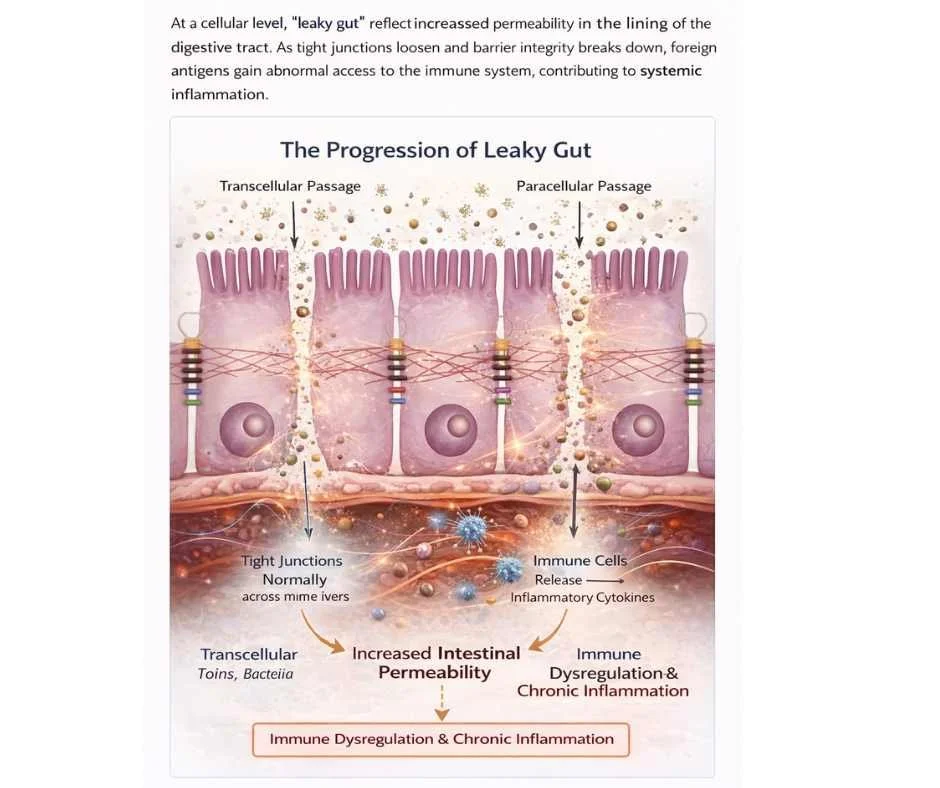
The Progression of Leaky Gut and Autoimmune Risk
In many individuals, increased intestinal permeability is associated with a recognizable pattern of immune escalation rather than an abrupt onset of autoimmune disease. This progression reflects the gradual loss of immune tolerance as the gut–immune interface becomes increasingly dysregulated.
1. Food Sensitivities and Immune Sensitization
Early immune activation often presents as delayed, non–IgE-mediated food reactions. These responses reflect immune sensitization to food antigens that cross the intestinal barrier due to increased permeability. Symptoms may be subtle at first—fatigue, joint stiffness, headaches, skin flares, or digestive discomfort—and are frequently dismissed or misattributed.
2. Environmental and Chemical Sensitivities
As barrier dysfunction and immune activation persist, the threshold for immune reactivity may lower. Sensitivity to chemicals, fragrances, molds, pollutants, and other environmental exposures becomes more common, reflecting broader immune dysregulation and impaired detoxification signaling.
3. Autoimmune Activation
With sustained antigen exposure and chronic immune stimulation, immune regulation may break down further. In genetically susceptible individuals, this can contribute to loss of self-tolerance, increasing the risk of autoimmune disease—defined by immune-mediated attack on the body’s own tissues (5).
This progression is not inevitable, but it underscores why early identification and targeted intervention matter. Addressing intestinal permeability and its drivers before immune tolerance is significantly impaired may reduce the likelihood of downstream autoimmune and inflammatory disease.
How To Heal Leaky Gut Naturally and Restore Gut Barrier Function
Healing leaky gut involves far more than temporarily reducing digestive symptoms. Effective recovery requires restoring gut barrier integrity, reducing chronic inflammation, recalibrating immune signaling, and identifying the upstream factors that continue to disrupt intestinal permeability over time.
From a functional medicine perspective, healing the gut is not a single supplement, elimination diet, or short-term protocol. Intestinal repair is a dynamic, systems-based process influenced by immune regulation, microbiome balance, nervous system function, metabolic health, environmental exposures, and nutrient status. Because these systems are closely interconnected, durable improvement typically depends on addressing the primary drivers sustaining inflammation and barrier dysfunction rather than masking symptoms alone.
Personalized Nutrition for Gut Healing and Reduced Inflammation
Nutrition plays a central role in restoring intestinal barrier function and reducing chronic inflammatory signaling. Personalized dietary strategies may focus on removing inflammatory foods, stabilizing blood sugar, improving nutrient density, and reducing immune-reactive exposures that aggravate gut permeability.
In many individuals, reducing ultra-processed foods, refined sugars, industrial seed oils, alcohol, and highly inflammatory dietary patterns may help decrease inflammatory burden and support epithelial repair. Depending on the individual, temporary removal of specific trigger foods—such as gluten or other immune-reactive foods—may also be appropriate while the gut lining heals.
Gut Repair Nutrients and Microbiome Support
Targeted nutritional and microbiome support may help strengthen intestinal barrier integrity, support epithelial regeneration, and improve microbial balance when used appropriately. Rather than relying on generalized “gut healing supplements,” support is ideally selected based on individual physiology, tolerance capacity, inflammatory burden, and microbiome patterns.
Depending on the clinical picture, gut repair strategies may focus on supporting short-chain fatty acid production, improving microbial diversity, calming inflammatory signaling, and restoring nutrients involved in mucosal repair and immune regulation.
Removing Ongoing Triggers That Damage the Gut Lining
Sustainable gut healing often requires reducing or removing the factors that continue to provoke inflammation and impair tight junction regulation. These contributors may include inflammatory foods, chronic stress, microbiome imbalance, medications, environmental toxins, alcohol, infections, mold exposure, or ongoing immune activation.
If these upstream triggers remain active, symptoms may temporarily improve while deeper barrier dysfunction and immune dysregulation persist underneath.
Stress Reduction and Nervous System Regulation
The gut and nervous system are deeply interconnected through the gut-brain axis. Chronic sympathetic activation, unresolved stress, elevated cortisol signaling, and autonomic imbalance may impair digestion, alter microbiome composition, reduce gut blood flow, and increase intestinal permeability.
For many individuals, nervous system regulation becomes an essential component of gut healing. Strategies that support parasympathetic tone and stress resilience may help reduce inflammatory signaling while improving digestive and immune function simultaneously.
Supporting Detoxification and Reducing Inflammatory Burden
Environmental toxins, oxidative stress, inflammatory cytokines, and impaired detoxification capacity may all contribute to ongoing gut barrier dysfunction. In some individuals, reducing toxic burden and supporting the body’s natural detoxification pathways may help decrease systemic inflammation and improve immune regulation.
This may involve addressing factors such as mold exposure, pesticides, plastics, heavy metals, poor air quality, or chronic inflammatory load that continue to stress the gut-immune interface.
Functional Medicine Testing for Leaky Gut and Intestinal Permeability
Advanced functional medicine testing may help identify the underlying factors contributing to intestinal permeability and chronic inflammation. Rather than focusing on symptoms alone, testing can help clarify which physiologic patterns are disrupting gut barrier integrity and sustaining immune activation.
Depending on the individual presentation, evaluation may include comprehensive stool testing, microbiome analysis, inflammatory markers, nutrient status, food immune reactivity, toxin burden, metabolic markers, or broader assessment of immune and digestive function.
This type of systems-based evaluation may help guide more personalized treatment strategies rather than relying on generalized protocols or trial-and-error approaches.
Testing may also help differentiate whether symptoms are being driven primarily by microbiome imbalance, inflammatory activation, food reactivity, environmental burden, or broader immune dysregulation.
→ Advanced Functional Lab Testing
Herbal Medicine and Acupuncture for Gut-Immune Regulation
Herbal medicine and acupuncture can play an important role in supporting gut healing, immune regulation, nervous system balance, and inflammatory control as part of a comprehensive, systems-based treatment approach (6–8). Because intestinal permeability is closely connected to autonomic function, immune signaling, stress physiology, circulation, and inflammatory tone, therapies that help regulate these systems may support broader recovery beyond digestion alone.
Acupuncture may help support parasympathetic nervous system activity, improve stress resilience, influence gastrointestinal motility, and modulate inflammatory signaling pathways involved in gut-immune communication. Herbal medicine may also be used strategically to support microbiome balance, mucosal integrity, digestive function, immune regulation, and inflammatory control depending on the individual clinical picture.
Rather than functioning as isolated symptom-based therapies, acupuncture and herbal medicine are often integrated within a broader functional medicine framework designed to support long-term physiologic regulation and restoration of gut barrier integrity.
Importantly, healing leaky gut does not require addressing every possible contributor simultaneously. Recovery is often most effective when the primary drivers sustaining intestinal permeability are prioritized strategically, response is monitored over time, and treatment evolves as gut barrier function, immune balance, and systemic regulation improve.
Why Leaky Gut Treatment Must Be Personalized
Leaky gut does not develop from a single isolated cause, and it rarely resolves through a one-size-fits-all approach. Increased intestinal permeability is typically the downstream result of multiple interacting stressors that differ significantly from person to person.
For some individuals, the primary drivers may involve gluten exposure, inflammatory foods, microbiome imbalance, chronic infections, or unresolved digestive dysfunction. For others, nervous system dysregulation, chronic stress, metabolic instability, environmental toxin exposure, mold illness, immune activation, or impaired detoxification capacity may play a more significant role. In many cases, several of these mechanisms are active simultaneously and continuously reinforce one another.
Because the intestinal barrier is closely connected to the immune system, endocrine signaling, mitochondrial function, detoxification pathways, and the nervous system, meaningful healing requires identifying which factors are most responsible for sustaining inflammation and barrier disruption in a given individual.
Applying generalized “gut healing” diets, supplements, or protocols without understanding these deeper physiologic patterns often leads to incomplete improvement, symptom recurrence, or stalled progress. A personalized, systems-based approach instead focuses on identifying the dominant drivers affecting gut barrier function and addressing them in a strategic sequence that supports long-term regulation and resilience rather than temporary symptom relief alone.
Personalized Gut Health Support
Chronic inflammation, autoimmune symptoms, fatigue, and persistent, unexplained health concerns are often evaluated in isolation. When gut barrier dysfunction and immune dysregulation are contributing factors, symptom-focused care alone is rarely sufficient.
At Denver Sports & Holistic Medicine, care is grounded in a root-cause, systems-based framework. Evaluation focuses on identifying the specific drivers of intestinal permeability and immune activation—such as dietary triggers, microbiome imbalance, inflammatory burden, stress physiology, or environmental exposures—and addressing them through an individualized plan designed to support durable healing rather than short-term symptom control.
→ Gut Health & Digestive Restoration
You may request a free 15-minute consultation with Dr. Martina Sturm to review your health concerns and outline appropriate next steps within a root-cause, systems-based framework.
Key Takeaways About Leaky Gut Syndrome
Leaky gut syndrome refers to increased intestinal permeability, where the gut barrier becomes less effective at regulating what enters circulation.
Symptoms may include fatigue, bloating, food sensitivities, brain fog, joint pain, skin issues, headaches, autoimmune flares, and histamine reactions.
Common drivers include gluten exposure, dysbiosis, chronic stress, inflammatory foods, medications, low vitamin D, environmental toxins, and immune dysregulation.
Healing leaky gut requires restoring gut barrier function, reducing inflammation, supporting the microbiome, and addressing the root causes that sustain permeability.
A personalized, systems-based approach is often necessary because intestinal permeability rarely develops from one cause alone.
Frequently Asked Questions About Leaky Gut Syndrome
What is leaky gut syndrome?
Leaky gut syndrome refers to increased intestinal permeability, a condition in which the intestinal lining becomes less effective at regulating what passes from the digestive tract into circulation. When the gut barrier becomes compromised, inflammatory particles such as bacterial fragments, toxins, and incompletely digested food proteins may cross into the bloodstream and trigger immune activation and systemic inflammation.
Is leaky gut a real medical condition?
While “leaky gut syndrome” is not always used as a formal diagnosis in conventional medicine, intestinal permeability is a well-documented physiologic phenomenon supported by extensive research. Increased intestinal permeability has been associated with chronic inflammation, immune dysregulation, autoimmune disease, microbiome imbalance, and various gastrointestinal disorders.
What are the most common symptoms of leaky gut?
Common leaky gut symptoms may include bloating, gas, abdominal discomfort, food sensitivities, fatigue, brain fog, headaches, joint pain, skin problems, allergies, histamine intolerance, autoimmune flares, and chronic inflammation. Many individuals experience symptoms outside the digestive tract because the gut plays a major role in immune and inflammatory regulation throughout the body.
Can you have leaky gut without digestive symptoms?
Yes. Many people with leaky gut experience fatigue, brain fog, joint pain, skin conditions, allergies, hormone imbalances, or autoimmune symptoms without significant digestive complaints. Because intestinal permeability affects immune signaling and systemic inflammation, symptoms often appear in multiple body systems rather than the gastrointestinal tract alone.
What causes leaky gut syndrome?
Leaky gut typically develops from multiple overlapping factors rather than a single cause. Common contributors include gluten exposure, inflammatory foods, microbiome imbalance, chronic stress, infections, medications, environmental toxins, alcohol, nutrient deficiencies, mold exposure, and immune dysregulation. In many individuals, several factors interact simultaneously and perpetuate chronic inflammation and gut barrier dysfunction.
Can stress cause leaky gut?
Yes. Chronic psychological and physiologic stress may contribute to increased intestinal permeability through the gut-brain axis. Elevated cortisol levels and autonomic nervous system dysregulation can impair digestion, alter microbiome balance, reduce gut blood flow, and increase inflammatory signaling within the intestinal lining.
What foods can make leaky gut worse?
Highly processed foods, refined sugars, industrial seed oils, alcohol, artificial additives, and inflammatory dietary patterns may worsen gut inflammation and intestinal permeability in susceptible individuals. Gluten and other immune-reactive foods may also contribute to ongoing immune activation and gut barrier disruption in some people.
Is gluten linked to leaky gut?
Research suggests that gluten may increase intestinal permeability by stimulating zonulin, a signaling protein involved in regulating tight junction function within the intestinal lining. This relationship is well established in celiac disease and may also contribute to non-celiac gluten sensitivity and broader inflammatory gut conditions.
Can antibiotics and medications contribute to leaky gut?
Yes. Certain medications—including antibiotics, NSAIDs, proton pump inhibitors, corticosteroids, and hormonal contraceptives—may contribute to gut barrier dysfunction and microbiome imbalance. These medications can alter microbial diversity, impair epithelial integrity, and increase inflammatory signaling within the gastrointestinal tract.
Is leaky gut linked to autoimmune disease?
Increased intestinal permeability is strongly associated with immune dysregulation and autoimmune disease development. When the gut barrier becomes compromised, chronic exposure to inflammatory particles may strain immune tolerance mechanisms and contribute to autoimmune activation in genetically susceptible individuals.
Can leaky gut cause brain fog and fatigue?
Yes. Chronic inflammation, immune activation, microbiome imbalance, blood sugar instability, and impaired nutrient absorption associated with intestinal permeability may contribute to fatigue, low energy, poor concentration, headaches, and brain fog. The gut and brain communicate closely through immune signaling pathways and the gut-brain axis.
Can leaky gut affect hormones and metabolism?
Yes. Gut barrier dysfunction and chronic inflammation may influence insulin sensitivity, cortisol regulation, thyroid signaling, estrogen metabolism, and mitochondrial energy production. Because the gut is closely connected to endocrine and metabolic regulation, chronic intestinal inflammation can contribute to broader hormonal and metabolic dysfunction.
Can leaky gut be healed naturally?
The intestinal lining has significant regenerative capacity when the underlying drivers contributing to permeability are addressed appropriately. Healing often involves reducing inflammatory triggers, improving microbiome balance, supporting immune regulation, addressing chronic stress, restoring nutrient status, and supporting gut barrier repair through a personalized, systems-based approach.
How long does it take to heal leaky gut?
Healing timelines vary depending on the severity of intestinal permeability, the degree of chronic inflammation, microbiome status, environmental exposures, immune dysregulation, and consistency of treatment. Some individuals notice improvement within weeks, while others may require several months of targeted support for more durable physiologic recovery.
Do probiotics help with leaky gut?
Probiotics may be beneficial for some individuals by supporting microbial balance and immune regulation, but they are not a standalone solution for intestinal permeability. Effective gut healing often requires addressing broader contributors such as diet, chronic stress, inflammation, infections, medications, and environmental triggers alongside microbiome support.
When should someone seek professional support for leaky gut?
Professional evaluation may be helpful when symptoms are persistent, systemic, worsening, or associated with autoimmune disease, chronic inflammation, fatigue, food sensitivities, or complex digestive issues. A personalized, root-cause approach may help identify the primary mechanisms contributing to ongoing gut barrier dysfunction and guide more targeted treatment strategies.
Can leaky gut affect skin problems like eczema or acne?
Yes. Gut barrier dysfunction and microbiome imbalance may contribute to inflammatory skin conditions such as eczema, acne, rosacea, psoriasis, hives, and chronic skin irritation. Because the gut and immune system are closely interconnected, chronic inflammation originating in the gut may influence inflammatory signaling throughout the skin.
Still Have Questions?
If the topics above reflect ongoing symptoms or unanswered concerns, a brief conversation can help clarify whether a root-cause approach is appropriate.
Resources
Nutrients – Leaky gut syndrome and nutritional compounds that support intestinal barrier integrity
Trends in Food Science & Technology – Pathogenesis of celiac disease and other gluten-related disorders and mitigation strategies
Nature Reviews Immunology – Vitamin D and the immune system
Gut – Intestinal barrier function and its regulation by the immune system
Nature Reviews Rheumatology – Environmental triggers of autoimmune disease
Frontiers in Immunology – Herbal medicines and their role in immune modulation
Nature Reviews Gastroenterology & Hepatology – Gut microbiota and immune system interactions
Evidence-Based Complementary and Alternative Medicine – Effects of acupuncture on immune and inflammatory markers